Mpox
What is mpox?
Mpox (formerly known as monkeypox) is a viral disease caused by the mpox virus, which is related to the viruses that cause smallpox and cowpox, but not to chickenpox. Despite the name, “monkeypox,” the exact source of the virus remains unknown.
The first human case was recorded in 1970, and since then, mpox has been reported in countries across central and west Africa and, more recently, has spread globally, with major outbreaks occurring in 2022 and 2024.
While generally milder than smallpox, mpox typically causes a similar rash with milder symptoms. Severity and fatality rates vary depending on the strain: the clade II strain responsible for the 2022 global outbreak is rarely fatal, while the clade I strain circulating in central Africa carries a higher risk of serious illness and death, particularly in children and people with weakened immune systems.
On this page, you can explore how mpox spreads, who is at risk, what the symptoms are, how to prevent mpox, and information on mpox outbreaks.
The first human case was recorded in 1970, and since then, mpox has been reported sporadically in some countries.
How does mpox spread?
Mpox spreads through close, direct contact. The most common ways include:
- Skin-to-skin contact with the rash, blisters, scabs, or bodily fluids of a person who has mpox, including during intimate or sexual contact
- Contaminated materials such as bedding, clothing, or towels that have been used by someone with mpox
- Infected animals through bites, scratches, or handling, particularly in parts of central and west Africa
- Pregnancy and childbirth, mpox can pass the virus to a fetus or newborn
Mpox does not spread easily through the air. Casual, brief contact, such as passing someone in a hallway or being in the same room, is not considered a significant risk for transmission.

Anyone can contract mpox, although the illness is generally not life-threatening. However, certain groups may be at higher risk for severe illness, including:
- People with severely weakened immune systems
- Young children, especially those under 8 years of age
- People with eczema or other active skin conditions (such as psoriasis, burns, or impetigo), which can allow the virus to spread more easily across the skin
- Pregnant people
What are the symptoms of this disease?
The symptoms of mpox infection include:
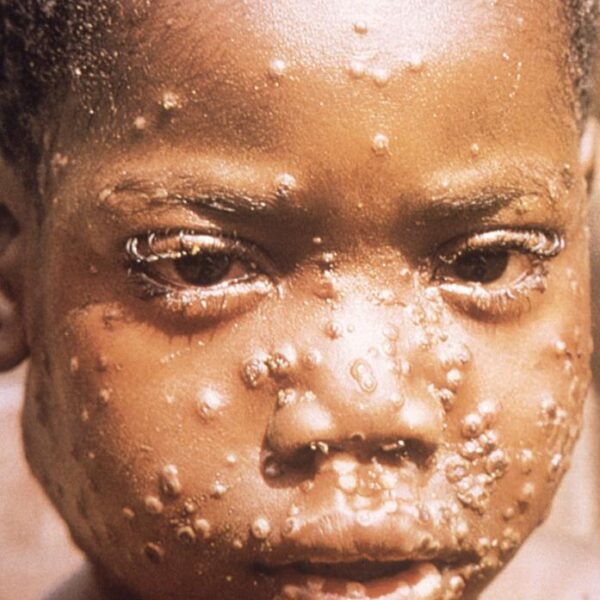
- People often get a rash that can look like pimples or blisters that appear on the face, inside of mouth, and on other parts of the body like hands, feet, chest, genitals, or anus. The rash is often painful before becoming itchy as it heals.
- Fever
- Headache
- Muscle aches and backache
- Swollen lymph nodes
- Chills
- Exhaustion
- Sore throat, nasal congestion, or cough
The illness typically lasts 2–4 weeks. Most people develop flu-like symptoms 1–4 days before a rash appears, though in some cases the rash comes first or flu-like symptoms may not appear at all.
How can I prevent this disease?
There are vaccines available to prevent mpox. The primary vaccine used in the United States is JYNNEOS, given as a 2-dose series 28 days apart. People at higher risk for infection are recommended to get vaccinated in consultation with their healthcare provider. The mpox vaccines can also prevent disease or reduce the severity of illness if given as soon as possible after exposure to an infected person, ideally within four days. Vaccination between 4 and 14 days after exposure may still reduce symptoms, but may not prevent disease.
Who is at higher risk of being infected by this virus?
- Those identified by public health officials as a contact of someone with confirmed mpox
- Those who had contact with someone who had a rash that looks like mpox or someone who has been diagnosed with mpox
- Those who had more than one sexual partners in the past 6 months in an area with known mpox
- Those who have jobs that may expose them to orthopox viruses, such as research laboratory workers who directly handle orthopoxvirus samples, and some designated healthcare or public health workers
How common are mpox outbreaks?
Mpox has caused two major global outbreaks in recent years, both of which led the World Health Organization (WHO) to declare public health emergencies of international concern. The first began in 2022, when mpox spread rapidly across many countries that had not previously reported cases, including the United States. That outbreak was caused by a strain called clade IIb and primarily affected men who have sex with men. A strong public health response, including vaccination and community outreach, controlled the outbreak in 2023. Low-level transmission of clade IIb continues in the United States and globally.
A second, more serious outbreak emerged in 2024, driven by a different and more transmissible strain called clade Ib, which originated in the Democratic Republic of the Congo and spread to neighboring African countries before reaching other parts of the world, including the United States. Unlike the 2022 outbreak, clade Ib has been spreading through both sexual and non-sexual close contact, including household transmission.While many of those affected in these outbreaks were men who have sex with men, anyone who has been in close contact with someone who has mpox can get the illness.
To learn more about current mpox outbreaks and spread, visit CDC’s Mpox in the United States and Around the World: Current Situation web page.
Immunization Schedules
To ensure that your family is up to date on their vaccines, view or download the childhood and adult immunization schedules and talk to your healthcare provider.


