Laith
An RSV Story
Place of Residence: San Francisco, California
Jessica’s family was enjoying the winter holidays when her son, Laith, came down with respiratory syncytial virus (RSV). What started as cold-like symptoms quickly escalated into a five-day hospital stay.
Jessica shares her family’s frightening experience with RSV below.
How would you describe Laith? What was he like as a baby?
Laith is my second-born, and he’s my only son. From the moment he was born, he was the most affectionate, tender, sweet, and cuddly boy. He was huge—he was my biggest baby at over 9 pounds—but the post-partum season with him was heaven because he was so lovely to hold and breastfeed.
He’s now a very energetic, athletic, sports-obsessed boy who’s really good at reading and math.
When did Laith get sick with RSV? How did you know he wasn’t feeling well?
I remember it quite vividly. It was Christmas time in 2019, and my parents were in town. My son had symptoms that I thought were just a cold. He had been down for a nap and was just waking up, so his door was open. My oldest child is about 2 years older than him, and she went into his room and said, “Mama, Laith is in trouble.”
My daughter wasn’t even four years old at the time; I don’t even know how she had the discernment or ability to tell that her brother was in distress. But every hair on my body stood up, every maternal instinct I had was activated, and I ran into his room.
I picked him up, and I could tell that he was working too hard to breathe. My daughter had needed a couple of breathing treatments before, so I was familiar with the signs and could recognize when a kid might need a nebulizer. So, in my mind, I thought Laith probably needs to go to the pediatrician, and they can do a breathing treatment. I called the after-hours nurse, and she recommended that we come in. I walked into their office thinking, we’ll be back home in a few hours, he’ll have a nebulizer, and he’ll be okay.
 While we were in the doctor’s office getting the treatment, our pediatrician very calmly put her hand on my knee and said, “I don’t want to scare you, but we are going to call an ambulance.” In that moment, all the blood rushed out of my head, and I felt like I was going to faint. I responded, “What do you mean? I thought we were doing the breathing treatment, and it looked like it was working.” But his oxygen saturation level was low, and he was still working too hard to breathe.
While we were in the doctor’s office getting the treatment, our pediatrician very calmly put her hand on my knee and said, “I don’t want to scare you, but we are going to call an ambulance.” In that moment, all the blood rushed out of my head, and I felt like I was going to faint. I responded, “What do you mean? I thought we were doing the breathing treatment, and it looked like it was working.” But his oxygen saturation level was low, and he was still working too hard to breathe.
Our pediatrician explained to me what would happen next, saying that the paramedics would come, put me on the gurney, then put Laith on top of me on the gurney, and I would ride with him to the children’s hospital. Everything after that felt like it was moving in slow motion. The paramedics came, did what our pediatrician said they would do, and we had a very uneventful ride to the hospital. I was sobbing the whole time.
As they pulled us out into the waiting room, there was a mom who looked at me and said, “We’ve been there. You’ll be fine.” It was a really sweet, human moment, where this woman looked at me and Laith and basically said: this sucks, but he’s going to be okay.
In the emergency room (ER), my husband and I thought my son might just need another treatment and then be sent home, but they told us he needed to be admitted. Our family had never experienced a hospital admission, so I remember thinking, what does this mean? The doctor there said he would need to be monitored on supportive oxygen until his oxygen saturation level improved.
During all this, Laith still seemed like my son, but he looked uncomfortable and sad. Even though everything escalated so quickly, there was never a moment when I thought he was dying—at least I didn’t let my mind go there. I knew he needed more care, but I kept feeling shocked by how the situation unfolded.
I am an infectious disease epidemiologist, so I feel like I’m a medically literate person. I understand a lot of information adjacent to what my son was experiencing, but I still felt powerless. Even if in my head I knew the progression of how a virus would work in a body, I felt completely helpless. My son's hospitalization humbled me to the max.
How did his illness progress?
Laith ended up spending five days and four nights in the hospital, which is a pretty long stay. He got better each day, but those first few days his oxygen saturation was not at a level where they felt comfortable discharging him. They were worried about him regressing at home and then having to come back.
The care team told us that we weren’t alone—there were so many children in the hospital and intensive care unit (ICU) because of respiratory viruses. They connected us with the pulmonologist, and the respiratory therapy team came in and explained what the treatment device was going to be like. They put Laith in a special crib that had every tube you can imagine. He was on oxygen through his nose, and they placed an IV as back up if he needed it. We had to treat his room as a quarantine, so we were all in masks, gloves, and gowns. It wasn’t until the third day that they allowed us to drop those precautions.
Laith did alright, but I don’t think I slept a minute any of those nights. My husband and I took turns for the overnights, but I typically just watched him as he slept all night. I kept waiting for inconsistencies in the beeping from his monitors, waiting for a moment when a signal went off. The care team was coming in every few hours to check on him and take vitals. I always asked them if he was okay.

There is nearly a 100% chance that your kid is going to get RSV, and you just don’t know if they’re going to get it severely or not.
How was Laith’s recovery?
Eventually, Laith tested positive for RSV, but the doctor said the diagnosis didn’t change the treatment. We were thankful that Laith never developed pneumonia or had any acute complications. When he was strong enough to sit up, I remember watching him chomp on crackers and thinking, oh, he’s coming back to us.
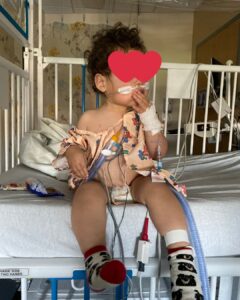 Around the fourth day, the care team allowed my parents to visit. The team was starting to talk about discharging Laith, as long as he did well overnight and was consistently well in the morning. We ended up being discharged the next day, which was New Year’s Eve, and all I wanted to do was be home with my healthy babies and end 2019.
Around the fourth day, the care team allowed my parents to visit. The team was starting to talk about discharging Laith, as long as he did well overnight and was consistently well in the morning. We ended up being discharged the next day, which was New Year’s Eve, and all I wanted to do was be home with my healthy babies and end 2019.
I never could have expected what would happen in 2020. Laith’s hospitalization occurred three months before the COVID-19 pandemic, so when COVID-19 emerged, I had such a deep trauma response to it. I remember thinking, “I just saw my son on supportive oxygen—I am not going to do that again.” Because of our experience with RSV, I had an extremely low risk tolerance for COVID-19. We still play it fairly safe with COVID-19, because once you experience your kid needing oxygen, you don’t ever want to go through that again.
When we went back to the pediatrician about a week later for a check-up, Laith was totally fine; he fully recovered and didn’t have any damage or impairments. We were really, really lucky. I think his age helped, because at that point my son was 19 months old. Usually, it’s children who are one year old or younger who are most at risk for an RSV hospitalization.
How did Laith’s illness impact your family?
Laith’s hospitalization was really hard on my parents. They were completely sick to see him so unwell. When they visited him in the hospital, I asked them not to show how visibly distraught they were because Laith was getting stronger and recovering. I have really sweet memories of them holding his hand and smiling and laughing with him.
I am the emotional one in my marriage, so I was usually the one with the wet face. But my husband was also very scared because we’d never experienced anything like that. We’d only been parents for a few years. Now that I have three kids, things are not as scary, but your first hospitalization is a really intense core memory. It trauma-bonded me and my husband.
I’ve heard parents talk about having to carry two worlds when you’re dealing with a traumatic event like a hospitalization. It was so important for us to try and keep things as normal as possible for our oldest child, who was still a toddler. She didn’t understand why her brother wasn’t coming home to sleep in his bed. My husband and I would spend time with her in shifts, and he suggested I take her ice skating. I remember thinking, how can I go ice skating when my son is in the hospital? But we also had a daughter to take care of, and she wanted to go.
How did your experience with Laith’s hospitalization impact you moving forward?
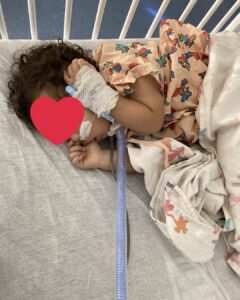 Laith’s experience with RSV impacted my parenting. I always tried to be risk-averse, and we were very cautious during the COVID-19 pandemic. Laith’s illness had a lingering, residual impact on the decisions we made for our family.
Laith’s experience with RSV impacted my parenting. I always tried to be risk-averse, and we were very cautious during the COVID-19 pandemic. Laith’s illness had a lingering, residual impact on the decisions we made for our family.
When I was pregnant with my third child, the maternal RSV vaccine wasn’t available yet, nor were the monoclonal antibodies when she was born. Both prevention options were approved a year later. At that point, she was no longer eligible.
She got sick during her first winter, and she came back positive for RSV. Getting a positive RSV test on my third kid was a bit triggering, even though she was doing okay. I remember thinking, I can’t do this again.
Thankfully, she fared much better, but that’s how prolific RSV is. Almost every kid gets it by the time they turn 2. It wasn’t shocking that she got it; it was more of a welcome relief that she didn’t get it so severely.
What would you tell new moms who are considering RSV prevention options for their baby?
Every day, I wish I could go back in time with the RSV protection tools that are now available. All of my family’s heartache, pain, and suffering could have been prevented. I’ve had many friends who have had babies within the last couple of years, and it is, without a doubt, one of the first things I say: if you’re going to give birth around respiratory virus season, please don’t skip this one. There is nearly a 100% chance that your kid is going to get RSV, and you just don’t know if they’re going to get it severely or not. It’s not worth the risk.
The statistics are shocking—most hospitalizations for children under 5 are from RSV, most children will get the virus, and these RSV prevention options are so effective that they essentially take away the risk. I have a friend who is a pediatric critical care doctor in Washington, D.C., and she told me that they barely saw RSV last season. The virus used to overwhelm their emergency room. RSV prevention options are nothing short of a miracle.
If there are parents who are on the fence, I want to clarify that RSV monoclonal antibodies are not a vaccine for babies. The antibodies are created from people who have recovered from RSV, and it’s a dose of protection given directly to the body. You don’t even have to wait two weeks for your baby’s body to build protective antibodies on their own. Your baby essentially receives a ready-made protective shield against a really nasty disease.
RSV doesn’t discriminate. I am a healthy person with healthy kids. My son didn’t have any preexisting health conditions, and he wasn’t immunocompromised. I never could have known he would need to be hospitalized with RSV, nor could any of his doctors.
When we were in the hospital, I remember thinking, when are they going to get a vaccine for this? RSV isn’t flu, it isn’t a regular cold—surely we could do something to protect children from this virus. And now, we can.
BECOME A VACCINE ADVOCATE
There are lots of ways you can make a difference in your community.

